Dollars and sense: Saving teeth vs. placing implants
The long-term success rate of dental implants has been well-documented in the literature1 and is a technology that has been a boon to the financial element of dentistry. Similarly, retention of teeth with moderate to advanced bone loss via various periodontal treatment methods has enjoyed similar to higher long-term success rates.2 The practitioner often relies on clinical experience and therapeutic familiarity when deciding whether to extract periodontally involved teeth and replace with dental implants vs. saving the natural dentition with regenerative or resective therapy. A relatively new concept, however, that should be incorporated into this decision matrix is the long-term cost effectiveness to the patient when comparing treatment modalities.
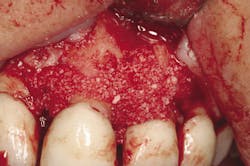
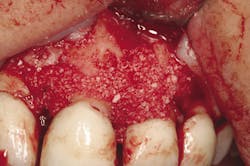
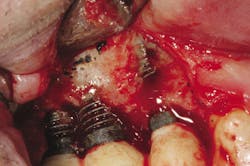
Retention of periodontally compromised teeth with initial, surgical, and supportive therapy has been shown to have high long-term success rates in the literature.3,4 Typical periodontal treatment for patients with moderate to advanced disease when first presenting to a dental office can consist of quadrant scaling and root planing, osseous surgery with or without regenerative therapy (Figs. 1 and 1a), and supportive periodontal maintenance at specific intervals. Estimated totals for this type of "start-up" treatment are in the range of $2,000 to $4,000 depending on geographic location (see Table A). This treatment, if maintained by the patient with diligent home care, has proven to be effective in terms of the prevention of further periodontal progression and tooth retention over a long-term period.5
When analyzing the cost to maintain this start-up treatment via supportive periodontal therapy with maintenance intervals of three to four times a year with or without local adjunctive antibiotics, dollar amounts range from $500 to $1,000 a year, again dependent upon geographic location. In a small subset of the population (less than 5%), periodontal disease can reoccur after treatment, excluding those patients who demonstrate blatant noncompliance with home care, and treatment will have to be rendered again, increasing the overall costs of this type of therapy.6
Although implants have typically enjoyed high long-term survival rates,7 their associated initial financial impact is much higher than that of saving the natural dentition.8 Conservative valuations place start-up costs for implant treatment around two to three times higher than saving natural dentition via periodontal therapy (Table 2). In addition, implants are not without complications, and both biologic and/or mechanical complications can be associated with additional treatment costs to the patient. Recently, the literature has been replete with discussion of biologic complications in the form of peri-implant disease. Peri-implant diseases fall into two categories: peri-implant mucositis and peri-implantitis.
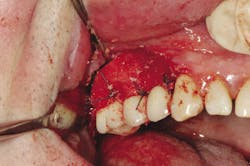
The term peri-implant mucositis describes a reversible inflammatory reaction in the mucosa adjacent to an implant,9 a term that has become known as implant gingivitis. Typical treatment involves quadrant scaling and root planing with implant-friendly armamentarium. The literature also has shown that mechanical debridement in conjunction with systemic and/or local antibiotic placement has increased the efficacy of this type of treatment10, but it can obviously be associated with higher treatment costs (Fig. 2). Studies show that the prevalence of peri-implant mucositis can be as high as 50% to 80% of implants in function.11 Peri-implantitis has been defined as an inflammatory process that affects the tissues around an osseointegrated implant in function and, like periodontitis, results in loss of supporting bone.
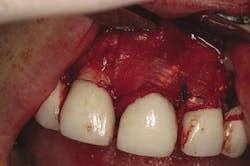
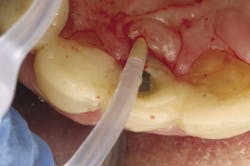
Clinical treatment of this disease is often determined by severity, but in general often includes flap surgery, bone grafts, membranes, growth factors, and/or soft-tissue grafts12 (Figs. 3 and 3a). The overall financial impact upon the patient for this type of treatment can be quite high considering the patient was already subject to initial start-up costs of treatment. (Table C). In addition, maintenance intervals after implant therapy should be equal to if not more stringent than those of natural teeth. The prevalence of peri-implantitis has been shown in some studies to range from 11% to as high as 47% of implant sites analyzed.13 A large disparity in percentages can be seen when comparing the prevalence of reoccurring periodontal disease after treatment vs. the percentage of implants that will demonstrate complications after prosthesis insertion. With that said, studies show that periodontal therapy has proven to be cost effective when compared to other types of tooth replacement therapy over a 15-year period evaluation.14
The following tables present actual treatment cost differences between the patient opting to "save" the natural tooth (Treatment Plan A) vs. "removal" with extraction and implant (Treatment Plan B). These fees are dependent on geographic location and represent insurance codes from the New York City, Los Angeles, and Chicago areas.
Table 1
Treatment Plan A Periodontal Regeneration | New York City (10022) | Los Angeles (90003) | Chicago (60605) |
(D4261) Osseous surgery (flap & closure) | $950.00 | $1,000.00 | $873.00 |
(D4263) Bone replacement graft | $475.00 | $558.00 | $500.00 |
(D4265) Biologic materials (Enamel Matrix Derivative) | $350.00 | $399.00 | $190.00 |
(D4266) Guided tissue regeneration | $400.00 | $525.00 | $500.00 |
(D4910) Periodontal maintenance | $195.00 | $150.00 | $132.00 |
GRAND TOTAL COST & TIME INVESTED | $2,370.00 1-3 hours | $2,632.00 1-3 hours | $2,195.00 1-3 hours |
Table 2
Treatment Plan B Extraction and Implantation | New York City (10022) | Los Angeles (90003) | Chicago (60605) |
(D7140) Extraction, erupted tooth or exposed | $300.00 | $157.00 | $160.00 |
(D7953) Bone graft (not same-day implant placement) (D6104) Bone graft (at time of implant) | $450.00 | $455.00 | $450.00 |
(D4266) Guided tissue regeneration | $400.00 | $525.00 | $500.00 |
(D6010) Surgical placement (implant body) | $2,250.00 | $2,118.00 | $2,000.00 |
(D6057) Custom-fabricated abutment | $975.00 | $750.00 | $750.00 |
(D6059) Abutment-supported implant crown (HN) | $1,850.00 | $1,500.00 | $1,404.00 |
(D4910) Periodontal maintenance | $195.00 | $150.00 | $132.00 |
GRAND TOTAL COST & TIME INVESTED | $6,420.00 3-9 months | $5,655.00 3-9 months | $5,396.00 3-9 months |
Table 3
Treatment Plan C Peri-implantitis Surgery | New York City (10022) | Los Angeles (90003) | Chicago (60605) |
(D6100) Implant removal (by report) | $500.00 | $475.00 | $500.00 |
(D6101) Debridement peri-implant defect | $350.00 | $200.00 | $350.00 |
(D6102) Debridement/osseous peri-implant defect | $475.00 | $375.00 | $450.00 |
(D6103) Bone graft repair/peri-implant defect | $675.00 | $550.00 | $675.00 |
(D6080) Implant maintenance procedures | $300.00 | $150.00 | $275.00 |
COST FOR PRIOR IMPLANT PLACEMENT | $6,420.00 | $5,655.00 | $5,396.00 |
GRAND TOTAL COST & | $8,720.00 1-2 years | $7,405.00 1-2 years | $7,646.00 1-2 years |
This information was presented to a real patient in a private practice setting along with long-term survival rate percentages of each of the comparative treatments. After reviewing the survival rates as well as the financial costs in relation to each treatment plan, the patient accepted Treatment Plan A, citing the following reasons: desire to keep her own teeth, less cost, and quicker time to completion.
Another real scenario that took place in a private practice with actual dollar amounts can be seen with Table 3. A patient had already paid for treatment in Table 2 in the $5,000 to $7,000 range and presented to the office with moderate peri-implantitis. In addition to the invested money, she was now going to be responsible for the dollar amounts shown in Table 3.
After reviewing the additional costs and lengthy healing time involved with surgery to correct the ailing implant, the overall costs associated with treatment were in the $8,000 to $9,000 range with more than three years of treatment time invested. Of important note is that most insurance companies limit the amount of reimbursement for implant-related services. Accurate ADA coding and submissions when dealing with insurance companies must occur in order to facilitate services and expedite reimbursements.
In conclusion, when deciding between saving the natural dentition and extracting and placing implants, there are many factors to consider. In addition to long-term success rates, the practitioner and the patient need to consider the long-term economic impact the patient will endure. Both implants and periodontal therapy to save natural teeth have high initial success rates with implants usually demonstrating higher start-up costs. However, when looking at long-term retention rates, teeth often demonstrate fewer complications and have less of a financial impact when correction is needed.
References
1. Simonis et al. Long-term implant survival and success: A 10-16-year follow-up of non-submerged dental implants. Clin Oral Implants Res. Jul. 2010;21(7):772-777.
2. Carnevale G, Di Febo G, Tonelli MP, Marin C, Fuzzi M. A retrospective analysis of the periodontal-prosthetic treatment of molars with interradicular lesions. The International Journal of Periodontics & Restorative Dentistry 1991;11:189-205.
3. Hirschfeld L, Wasserman B. A long-term survey of tooth loss in 600 treated periodontal patients. J Periodontol. 1978;49:225-237.
4. Oliver RC, Brown LJ, Loe H. Periodontal diseases in the United States population. J Periodontol. 1998;69:269-278.
5. Axelsson P, Lindhe J, Nyström B. On the prevention of caries and periodontal disease. Journal of Clinical Periodontology, 1991;18:182-189.
6. Magnusson et al. Refractory periodontitis or recurrence of disease. J Clin Periodontol. Mar. 1992;23(3 Pt 2):289-292.
7. Simonis P, Dufour T, Tenenbaum H. Long-term implant survival and success: A 10-16-year follow-up of nonsubmerged dental implants. Clin Oral Implants Res. Jul. 2010;21(7):772-777.
8. Schwendicke F, Graetz C, Stolpe M, Dörfer CE. Retaining or replacing molars with furcation involvement: A cost-effectiveness comparison of different strategies. J Clin Periodontol 2014; 41:1090-1097.
9. Albrektsson T, Isidor F. Consensus report of session IV. In: Lang NP, Karring T, ed. Proceedings of the First European Workshop on Periodontology. London: Quintessence, 1994: 365-369.
10. Salvi et al. Adjunctive local antibiotic therapy in the treatment of peri-implantitis II: Clinical and radiographic outcomes. COIR 2007;18:281-285.
11. Lindhe J, Myle J. Peri-implant diseases: Consensus report of the Sixth European Workshop on Periodontology. J Clin Periodontology 2008;35(suppl 8):282-285.
12. Froum SJ, Froum SH, Rosen PS. Successful management of peri-implantitis with a regenerative approach: A consecutive series of 51 treated implants with a 3- to 7.5- year follow-up. IJPRD 2012;32(1):1-20.
13. Koldsland O et al. Prevalence of peri-implantitis related to severity of the disease with different degrees of bone loss. J Perio Feb. 2010;81(2)231-238.
14. Pretzl B, Wiedemann D, Cosgarea R, Kaltsch-mitt J, Kim TS, Staehle HJ, Eickholz P. Effort and costs of tooth preservation in supportive periodontal treatment in a German population. Journal of Clinical Periodontology 2009;36:669-676.
Scott Froum, DDS, a graduate of the State University of New York, Stony Brook School of Dental Medicine, is a periodontist in private practice at 1110 2nd Avenue, Suite 305, New York City, New York. He is the editorial director of Perio-Implant Advisory and serves on the editorial advisory board of Dental Economics. Dr. Froum, a diplomate of the American Board of Periodontology, is a clinical associate professor at SUNY Stony Brook School of Dental Medicine in the Department of Periodontology. He serves on the board of editorial consultants for the Academy of Osseointegration's Academy News. Contact him through his website at drscottfroum.comor (212) 751-8530.
Kyle L. Summerford is CEO and founder of Summerford Solutions, Inc., and editorial director of PennWell's Dental Assisting Digeste-newsletter. He provides private business coaching for dentists. Mr. Summerford is a professional speaker focusing on topics such as increasing profits, staff etiquette training, and maximizing dental insurance benefits. He is a contributing author for Dental Economics, DentistryIQ, and Perio-Implant Advisory. Visit his website at www.ddsguru.com, available to dentists and team members for educational purposes, or contact him by email at KyleLSummerford@gmail.com with inquiries regarding his practice management consulting services.
About the Author

Scott Froum, DDS
Scott Froum, DDS, a graduate of the State University of New York, Stony Brook School of Dental Medicine (SUNY), is a periodontist in private practice in New York City. He is the editorial director of Perio-Implant Advisory and serves on the Dental Economics advisory board. Dr. Froum is a volunteer professor in the postgraduate periodontal program at SUNY, is a trained naturopath, and is the scientific director of Meraki Integrative Functional Wellness Center. Contact him at drscottfroum.com.
Read Dr. Froum's DE Editorial Advisory Board profile here.

Kyle L. Summerford
With more than 22 years of experience in dental, Kyle L. Summerford has a unique approach to case presentation and patient acceptance. As an OM and financial dental consultant, he leverages his knowledge to assist new and struggling dental practices. Through his education programs, Kyle empowers staff members with effective patient education skills and persuasion techniques. He has lectured at CE events and academic institutions. His expertise is further recognized through his column, Dental Coding with Kyle. He’s the founder of the Dental Office Managers Community. Visit his website at kylesummerford.com.